
Browse Ochsner's History
Start browsing through our timeline by selecting one of the decade buttons to the left.
After choosing a decade, select an icon at the bottom of the screen to view events in that timeframe.
Establishing the Ochsner Clinic
Local medical school professors Drs. Alton Ochsner, Edgar Burns, Guy A. Caldwell, Francis E. LeJeune, and Curtis Tyrone each contributed $4,300 of their own money to open the first private group practice clinic in New Orleans, similar to the models of the Cleveland Clinic and Mayo Clinic. While at a medical meeting in Ogden, Utah, Dr. Ochsner received the telegram from his partners that established the name as the Ochsner Clinic.
The physicians, surgeons and dentists of New Orleans expressed opposition to the new Clinic. They preferred their independent practices and felt a clinic setting was unfair competition.

Ochsner Clinic on Prytania Street Officially Opens
The first Ochsner Clinic opened at the corner of Aline and Prytania Streets in uptown New Orleans.

Alton Ochsner Medical Foundation Established
It quickly became apparent to the partners that their practice should aspire to create a permanent research, educational and charitable organization serving not only the people of the New Orleans area, but those of the Gulf South area as well.
Together with Mr. J. Blanc Monroe and Mr. Theodore Brent, the five partners became the founders of The Alton Ochsner Medical Foundation in 1944, a non-profit organization dedicated to the purposes of research, education and charity.
The initial step in the development of the Foundation's educational program was the establishment of Fellowship grants for advanced graduate training in various medical and surgical specialties.
At left: Alton Ochsner, M.D.

Ochsner Accepts First Class of Physician Graduates
In keeping with its mission to emphasize physician education, Ochsner accepted its first class of graduates in 1944. At that time, there were nine residents for internal medicine and surgery. In just two years that number had increased five-fold and by 1946 there were 47 fellows.
As a teaching hospital, Ochsner provided noon conferences for staff physicians and fellows in training to review cases.

Station Hospital at Camp Plauché Adapted to Become First Ochsner Foundation Hospital
The Foundation purchased the buildings and equipment of the Station Hospital at Camp Plauché from the War Assets Administration. Following adaptation to civilian usage, it became the 200-bed Ochsner Foundation Hospital.
It was affectionately known as "Splinter Village" among the nurses who would take off their shoes during the hot New Orleans summers and, as a result, often find splinters in their feet from the wood floors.
Ochsner Foundation Hospital Opens for Business at Camp Plauché
The base hospital included 53 frame buildings and just two private rooms. Though these temporary frame structures served incredibly well their intended purposes, the need for a larger, permanent and more specialized hospital was all too soon apparent.
By the time it closed in 1954, "Splinter Village" had served more than 36,000 patients. It also was one of the first hospitals in the Gulf South to offer a comfortable family waiting lounge where families were kept constantly informed of the patient's progress during the operation.
Far left: Splinter Village Recovery Room
Near left: Family Waiting Room
By the Numbers
- In the first nine years of the fellowship program, 210 graduate physicians from 36 states and 20 foreign countries have been trained in nine chosen specialties at Ochsner.
- The Foundation’s periodical of selected medical writings by staff members is mailed to a list of 16,000 physicians throughout the world.

Groundbreaking Begins for New Jefferson Highway Campus
Following a successful campaign for funds to erect a more permanent institution, construction began on the new Ochsner Foundation Hospital on a 22-acre tract overlooking the majestic Mississippi River in New Orleans.

Dr. Alton Ochsner Successfully Separates Conjoined Twins
Dr. Alton Ochsner led the team that performed a successful separation of conjoined twins at Splinter Village. Carolyn and Catherine Mouton, the children of Lafayette, La. Mayor and Mrs. Ashton Mouton, were joined at the spine at birth.

Ochsner Foundation Hospital Moves to Current Flagship Location
On June 12, 1954, Ochsner Foundation Hospital officially moved from Camp Plauche to its current flagship campus on Jefferson Highway.
Over five hours, 134 patients were moved from the old wood-frame quarters at Splinter Village to the new five-story, 250-bed, air-conditioned hospital.

New Buildings Open on Hospital's Jefferson Highway Campus
The Brent House Hotel, named for deceased AOMF Board of Trustees member Theodore Brent and constructed next door to the hospital, offered accommodation for long-term patients and their families, as well as the first physician offices at the new campus.
The Libby-Dufour residence housed nurses and physicians in training, allowing them to be close to the hospital.
At left: Brent House Hotel

Ochsner is First in Area with Medical Heliport
Ochsner was the first in the region to introduce a helicopter landing site on campus.

First Research Building Opens on Hospital Campus
The Founders of the AOMF envisioned the ideal modern physician as one with an “unrelenting fervor for experiment, subjecting his fondest theories and practices to the critical test of searching investigation.” Research and contributions to the advancement of science were vitally important to the Foundation.
The first research building (later named the Richard W. Freeman Research Building) opened on the hospital’s campus in 1959.
At left: Richard W. Freeman Research Building and Richard W. Freeman
By the Numbers
- In 1951-52, 10,491 patients were admitted to the hospital. 82% of these came from 48 states and 899 came from 57 foreign countries.
- In 1952, the average hospital stay was 9.55 days.
- In 1953, the ever-increasing staff numbered 67 full time specialists, 13 consultants, and 50 graduate physicians in specialty training.

Ochsner Suite Featured on Magazine Cover
A spacious suite at Ochsner Hospital was featured on the cover of the January issue of The Modern Hospital.

Ochsner Clinic Moves to the Ochsner Hospital Campus
The clinic’s location in Uptown New Orleans became problematic as the clinic staff lost valuable hours in transit and patients were inconvenienced.
The Ochsner Clinic joined Ochsner Foundation Hospital in a modern facility adjacent to the hospital. The shared location resulted in greater efficiencies by concentrating physicians, laboratories and hospital facilities at a single site. Patient volumes increased and the staff expanded.

Infectious Disease Specialist Added to Staff
Ochsner expanded its Internal Medicine Department by welcoming Dr. George A. Pankey to the Staff. Dr. Pankey was one of the first practicing Infectious Disease Specialists in Louisiana.

Cardiovascular Research Inspires New Techniques and Innovation
Medical research continued to thrive with the establishment of cardiovascular diagnostic laboratories, inspiring new techniques and innovations that paved the way for future coronary vessel surgeries, open heart surgeries, the first heart-valve replacement, pacemaker implants, heart transplants, and lung transplants.
These innovations allowed the next generation of physicians to reach new heights in cardiovascular medicine.

First Adult Kidney Transplant in Region Performed at Ochsner
The first successful adult kidney transplant in the Gulf South region was performed by Dr. Paul DeCamp, Dr. William Brannan and Dr. Mims Gage.
The patient was referred from Florida to Ochsner Clinic. His kidney worked for almost 30 years.
At left: Dr. Mims Gage

First Pediatric Kidney Transplant in Gulf South Takes Place at Ochsner
The first successful pediatric kidney transplant in the Gulf South region was performed by Dr. Paul DeCamp, Dr. William Brannan and Dr. Mims Gage.
Forty years later, this patient was a grandfather and doing very well.
At left: Dr. Mims Gage

Ochsner Performs First Heart Transplant in Region
Dr. John Ochsner performed the first heart transplant in the Gulf South region.

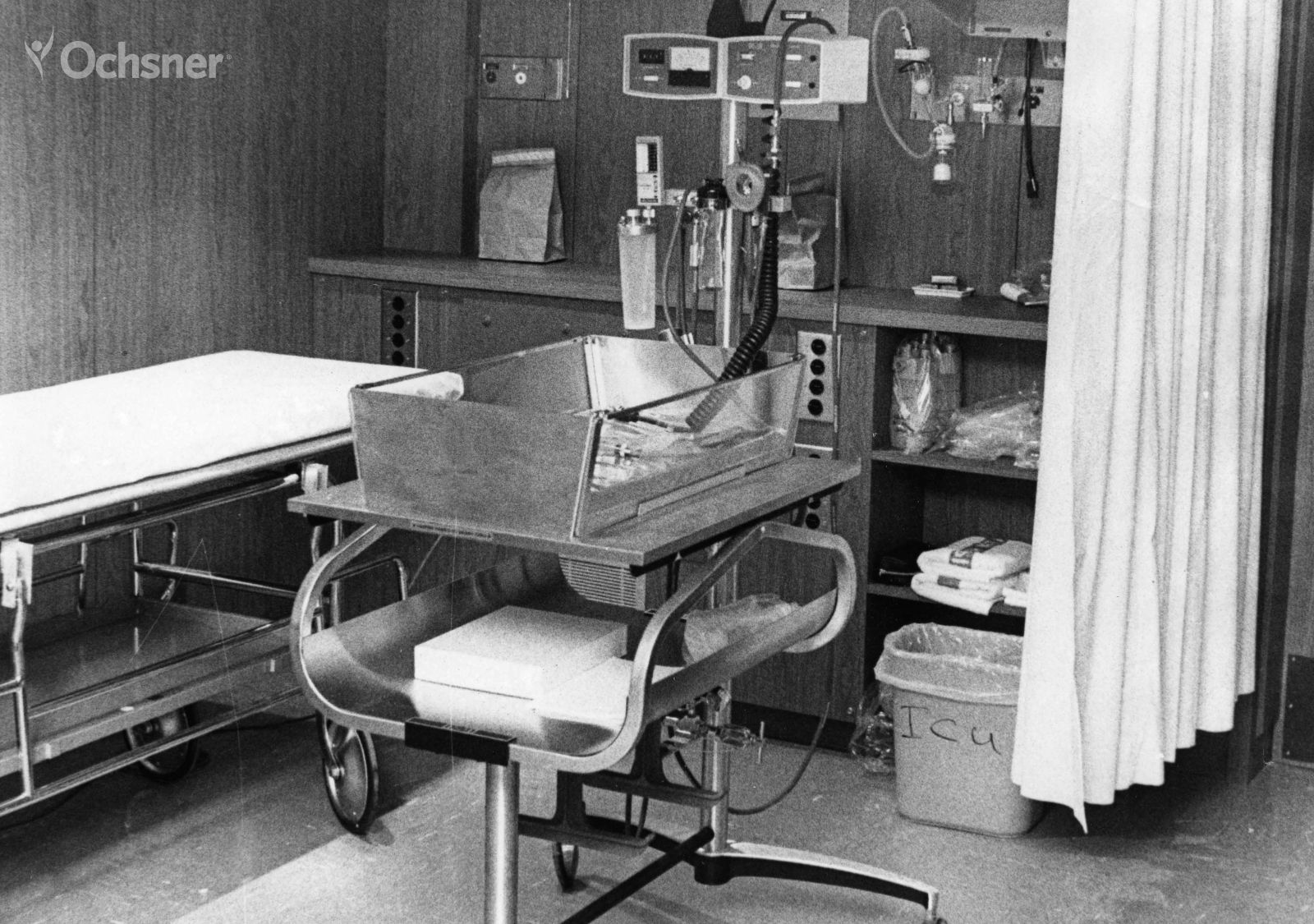
New Intensive Care Unit Opens
Ochsner's new Intensive Care Unit (ICU) opened in April 1972 and contained an infant cubicle. The ICU was the largest in the South.
Ochsner's Transplant Program Grows
Dr. John Ochsner implanted a heart pacemaker in the youngest patient ever. The 9-pound, 2-ounce recipient was only 18 hours old.
Ochsner’s first liver transplant later that year led to the growth of Ochsner Foundation Hospital’s multi-organ transplant program: liver, pancreas, lung, and heart-lung.
With these programs, Ochsner Foundation Hospital was recognized as a national leader in the field. Concomitantly, Ochsner played a large part in the creation and support of the Louisiana Organ Procurement Agency (LOPA).

Ochsner Physicians Invent Device to Close Hole in Heart Without Open-Heart Surgery
Dr. Terry D. King and Dr. Noel L. Mills invented an umbrella device that they implanted by catheter in the heart of a 17 year-old patient in 1975.
The King-Mills Umbrella Device, used for non-surgical closure of congenital interatrial septal defects, won the two Ochsner physicians the Young Investigator Award of the Cardiology Section of the American Academy of Pediatrics.

Ochsner Pioneers Neonatal Intensive Care Unit
The opening of Ochsner's Neonatal Intensive Care Unit (NICU), begun by Dr. Jay Goldsmith, made the hospital a leader in the NICU operation in the Gulf South region. It was a commitment on the part of Ochsner to treat its youngest and smallest patients with the same quality medical care available to their parents and grandparents.

Ochsner’s Graduate Medical Education Programs Develop Affiliations
Leonard J. Chabert Hospital opened in Houma, Louisiana as part of Louisiana’s charity hospital system. Under Dr. Frank Riddick’s leadership, Ochsner’s graduate medical education programs developed a strong affiliation with Chabert. This facility gave the residents learning opportunities to care for patients within the charity system.
With guidance and oversight from the Ochsner Clinic, South Louisiana Medical Associates was developed as a group practice that contracted with the State of Louisiana to provide senior staff supervision of hospital activities, patient care and medical education.
At left: Leonard J. Chabert Medical Center

By the Numbers
- In 1973, the Clinic recorded 500,000 patients.
- About 8.5% of those patients come from Central or South America.
- Referring physicians throughout the United States name Ochsner Clinic #1 in a survey by Medical Economics.
- Dr. Edgar Burns (at left) passed away on August 27, 1973 at the age of 78.
- By 1979, house staff has increased to 180.

Dr. Alton Ochsner Named DeBakey Surgical Award Recipient
Dr. Alton Ochsner became the second recipient of the Michael E. DeBakey Surgical Award. This honor is bestowed only on the world’s most outstanding surgeons for their significant contributions to surgery.
In 2000, Alton's son, Dr. John Ochsner, would receive the same award.
At left: Alton Ochsner, M.D. and his son, John Ochsner, M.D.

Last Surviving Ochsner Founders Pass Away
The institution mourned the deaths of Dr. Alton Ochsner who passed away on September 24, 1981 and Dr. Guy Caldwell who passed away on November 1, 1981. Dr. Curtis Tyrone passed away on July 13, 1982.
From left: Dr. Alton Ochsner, Edgar Saux, Dr. Frank Riddick, Dr. Merrill Hines, Dr. Curtis Tyrone, and (seated) Dr. Guy Caldwell.

Ochsner Cancer Institute Established
The Ochsner Cancer Institute was established in 1982. Utilizing a multidisciplinary approach to the treatment of cancer, this environment fosters innovation and collaboration.
In 1983, Ochsner joined the Community Clinical Oncology Program sponsored by the National Cancer Institute and represents the largest clinical trials network in Louisiana today.

Ochsner Augments Treatment Options for Newborns
The first infant was placed on extra corporeal membrane oxygenation (ECMO) at Ochsner. Ochsner’s ECMO program was the fourth initiated in the country.
By 1988, Ochsner had treated its 100th patient, further enhancing its national reputation as one of the leader centers for the treatment of high-risk newborns.

Ochsner Named Official World's Fair Healthcare Provider
Under the leadership of Dr. Michael Sullivan, Ochsner provided community outreach on a global stage by participating in the New Orleans World’s Fair. Ochsner showcased a 40-foot-high model of the human heart, pulsing with light to the accompaniment of the deep, slow sound of a heartbeat.
In addition, a 5,000-square-foot medical facility staffed by Ochsner physicians and nurses administered emergency medical care to the visitors attending the World’s Fair.

Ochsner Develops Integrated Care System to Provide Care from Hospital to Home
To further provide for the post-hospitalization needs of its patients, Ochsner inaugurated a home health services program and expanded its rehabilitation program in 1985.
These capabilities, along with the Ochsner Skilled Nursing Facility which went into operation in 1984, permitted Ochsner to offer its patients a full spectrum of Ochsner-quality care from the most intensive hospital-level care to recuperative support in the patient's own home.

Neighborhood Primary Care Clinics Open Around Greater New Orleans
Primary care services were emphasized and developed through a network of neighborhood clinics in Metairie, Kenner, West Bank and the North Shore, offering convenience and continuity of care to locations readily accessible to those we already serve. Ochsner also announced plans to extend to other areas of the Gulf South starting with the Ochsner Clinic of Baton Rouge.

Ochsner Health Plan Chartered - New Orleans' First Locally Owned and Managed HMO
Along with the development of the neighborhood primary care clinics, Ochsner Health Plan was chartered by Ochsner Clinic and Ochsner Foundation Hospital and offered prepaid care. This managed care method allowed the clinic patient base to expand, and health plan enrollment eventually exceeded 200,000 subscribers. When the Medicare program offered a prepayment option, Ochsner Health Plan incorporated this offering to accommodate the older generations of patients Ochsner served.

Ochsner Resumes Heart Transplant Program
Ochsner made headlines with the first of a rapid series of successful heart transplants. The resumption of heart transplants was sparked by new technologies in tissue-rejection control that have made transplants vastly more likely to succeed than they were 15 years ago when Ochsner pioneered the program in the south.

New Technology Enhances Patient Care
During the 1980s, Ochsner added new programs and technology, embracing innovation to enhance patient care. New services included bone marrow transplantation, magnetic resonance imaging (MRI), positron emission tomography (PET), gene therapy, and advanced chemotherapy.

By the Numbers
- In 1981, the 204 graduate physicians in training constitute one of America's largest non-university based programs, with an annual budget of over $5 million.
- In 1986, Ochsner medical institutions with more than 4,000 hospital, clinic, hotel and research center employees, rank as the second-highest employers in Jefferson Parish (after Avondale Shipyards).
- In 1986, the Alton Ochsner Award Relating Smoking and Health was established; the recipient receives a $15,000 award.
- In 1989, in just two and a half years, Ochsner Clinic of Baton Rouge has become the largest group medical practice serving the Baton Rouge region with almost fifty physicians offering care in more than two dozen specialties and subspecialties.
- In 1989, Ochsner Clinic staff was 290 physicians.

Ochsner Purchases Elmwood Fitness Center
Ochsner’s philosophy of encouraging health and wellness preventive care and commitment to a healthy community served as the impetus for the purchase of Elmwood Fitness Center.
Today known as Ochsner Fitness Center, there are four locations in the New Orleans area.

First After Hours Clinic Opens
The new Ochsner Clinic in Metairie housed Ochsner's first after-hours clinic, open at night, weekends and holidays to better serve patients. It offered space to expand Family Practice as well as to introduce a new section of General Internal Medicine.

Double Lung Transplant Performed on Youngest Person in U.S. History
In 1993, Ochsner surgeons performed a double lung transplant on the youngest person in U.S. history, and today Ochsner remains the only lung transplant program in Louisiana.

Frohlich Named Editor of Hypertension
Dr. Edward Frohlich was named editor of the prestigious American Heart Association Journal, Hypertension.
Dr. Frohlich joined Ochsner in 1976 as the Director of the Division of Research. Over the ensuing decades, his laboratory and clinical investigations, educational programs, and therapeutic innovations have kept Ochsner at the forefront of excellence in the management of hypertensive diseases.

Ochsner Further Expands its Reach
Ochsner further expanded its reach by adding major multidisciplinary satellite clinics throughout the region including Covington, Hammond, Lapalco, Rothschild Pediatrics, Tangipahoa, and Perkins and Mid-City in Baton Rouge.
Ochsner Rated One of the "Best Hospitals in America" by U.S. News
Ochsner Hospital was rated one of the “Best Hospitals in America” by U.S. News & World Report. The annual Best Hospitals rankings recognize hospitals that excel in treating the most challenging patients.
Ochsner would continue to be regularly ranked among the Best Hospitals in the country in numerous specialties -- by 2016, Ochsner had been named 16 times since 1996.

First Ochsner Journal Published
The Ochsner Journal is a quarterly publication designed to support Ochsner Health System's mission to serve, heal, lead, educate, and innovate. The Journal provides a wide range of peer-reviewed, timely and practical information for practicing physicians, healthcare professionals and physicians in training.

Ochsner Clinic and Alton Ochsner Medical Foundation Unify
Dr. Frank A. Riddick, CEO of the Alton Ochsner Medical Foundation, and Dr. Patrick Quinlan, CEO of Ochsner Clinic, dedicated two years of tireless work to negotiation between the parties.
On August 31, 2001, the clinic and the foundation agreed to consolidate into a single organization, the not-for-profit Ochsner Clinic Foundation, later designated the Ochsner Health System, with Dr. Patrick Quinlan as chief executive officer and a unified board from the predecessor organizations.
The unified organization with a single decision-making body and single management structure was viewed as essential to function and succeed in a changing medical and economic environment by eliminating duplicative and sometimes competing management, governing, and operating structures.

By the Numbers
- In 1991, building expansion of OMC- Jefferson Highway began with construction of over 600,000 square feet of new buildings and renovation of one million square feet of space.
- In 1992, Ochsner celebrated its 50th anniversary.
- In 1992, Ochsner hired 189 RNs and 39 LPNs.
Lieselotte Tansey Breast Center at Ochsner Opens
Named after benefactor Mrs. Lieselotte Tansey of Selle, Germany, the Breast Center is a multidisciplinary practice where patients can have tests, see their physicians, and rapidly obtain their diagnoses and treatment plan in one convenient location.
It is the only breast cancer program in New Orleans accredited by the National Accreditation Program for Breast Centers (NAPBC).

New Ochsner for Children Rapidly Becoming Benchmark for Innovative Pediatric Care in the South
The creation of Ochsner for Children brought together all existing pediatric functions under one umbrella, planning for expanding services, increasing medical staff and patient accessibility. It implemented a new vision of how medical care for children should be delivered.
As part of this vision, construction began at OMC- Jefferson Highway on a new 40,000 sq ft ambulatory center for children, as well as a PICU and NICU within the hospital.
Hurricane Katrina Makes Landfall near Slidell, LA
Hurricane Katrina was the costliest natural disaster, as well as one of the five deadliest hurricanes, in the history of the United States. The storm is currently ranked as the third most intense United States landfalling tropical cyclone, behind only the 1935 Labor Day hurricane and Hurricane Camille in 1969.
Hurricane Katrina Hits New Orleans - Ochsner Never Closes Its Doors
Ochsner was the area's only full-service hospital to remain completely functional during and after the storm. In addition, Ochsner Clinic provided the community's only Level 1 trauma care at its Elmwood facility after Hurricane Katrina's destruction of Charity Hospital.
Ochsner Acquires Three Local Hospitals To Ensure Healthcare Across the New Orleans Area
Ochsner secured the future of Memorial, Meadowcrest and Kenner Regional hospitals through an acquisition from Tenet Healthcare.
By the end of 2006, with the post-Katrina acquisitions of hospitals in Uptown New Orleans, in Kenner and on the West Bank, Ochsner Health System had grown to include seven hospitals, 21 health centers and eight specialized centers across South Louisiana.
Summit Hospital in Baton Rouge Joins Ochsner Health System
As the population in greater Baton Rouge continued to grow, specifically in Livingston Parish, having an expanded medical center like Ochsner just minutes away greatly benefited the region.
Summit Hospital became Ochsner Medical Center - Baton Rouge, a 201-bed hospital with over 280 physicians located near Livingston Parish. The Medical Center offered a comprehensive range of inpatient and outpatient services, including cardiopulmonary, emergency, robotic surgery, oncology, physical therapy and rehabilitation, radiology and imaging, as well as same-day surgery.
This growth also went hand in hand with the Baton Rouge Group Practice formed with Ochsner in 1986.

St. Anne General in Raceland Joins Ochsner Health System
Ochsner in New Orleans partnered with St. Anne General in Raceland to provide enhanced local care to patients served by the Lafourche hospital. This partnership enabled Lafourche residents to spend less time traveling and more time accessing healthcare in their own neighborhood. The hospital's new name became Ochsner St. Anne General Hospital.

Ochsner Again Recognized as a Magnet Hospital
For the second time, Ochsner Medical Center-Jefferson Highway was recognized as a Magnet Hospital by the American Nurses Credentialing Center. This designation is given to select healthcare organizations for quality patient care, nursing excellence and innovations in professional nursing practice.
Community Hospitals See Major Investments in Future
Investments at Ochsner Baptist Medical Center
The addition of 22 medical/surgical beds, a 3-bed intensive care unit, 2 endoscopy suites and a women's imaging center for mammograms and bone mineral density is part of a $22 million investment at this critical community facility.
Emphasizing Care for Mom and Baby
The newly-expanded labor and delivery unit at Ochsner St. Anne Hospital brought Ochsner-quality care to Louisiana's bayou communities. Also this year, Ochsner Medical Center - Kenner opened its NICU for premature babies and newborns, upgrades its labor and delivery unit with private rooms and continued practicing the latest birthing techniques.
Cardiovascular Services Expand at Ochsner Medical Center - West Bank
The Open Heart Surgery program reopened alongside a new strategic partnership with The Heart Clinic of Louisiana. Ochsner's West Bank facility became home to an infusion center offering local patients greater access to chemotherapy.

Kenner Neuroendocrine Tumor Program Is Among Largest In U.S.
Ochsner Medical Center - Kenner became home to a multidisciplinary neuroendocrine tumor program that is among the largest in the United States treating this extremely rare cancer.
In partnership with Louisiana State University, the program provides a multi-disciplinary, team-based approach with state-of-the-art diagnostics and has had nearly 16,000 clinic visits to serve its patients.

B.R. Hospital Is Global Robotic Surgery Leader
Performing more robotic gynecological surgeries than any other facility in the world, Ochsner Medical Center - Baton Rouge is one of only six global training sites for the da Vinci Robotic Surgical System.

Ochsner Transplant Institute Reaches Major Milestones
Ochsner's Transplant Institute performed its 1,000th liver transplant, 1,000th kidney transplant, and 700th heart transplant in 2007. At this time, the Institute scored in the 99th percentile in overall patient satisfaction and offered patients some of the shortest wait-list times in the nation. The median wait time in 2007 for liver transplants at Ochsner was just 35 days, compared to approximately 575 days nationally.
Care provided by the Institute includes addressing the emotional, financial and practical support issues so often faced by patients and their families.

Ochsner is Prepared as Hurricane Gustav Makes Landfall
Ochsner Medical Center Baton Rouge was the only healthcare provider to serve its community without interruption during and after Hurricane Gustav.
University of Queensland Ochsner Clinical School Opens
The University of Queensland Ochsner Clinical School opened with nine full-time medical students. All students went on to graduate from this innovative two-continent medical education program in December 2012 and began their residencies in July 2013. This first graduating class completed two years of study at The University of Queensland in Brisbane, Australia, followed by two years of clinical study at Ochsner.
The Ochsner Clinical School program continues to grow. In 2016, the fourth class graduated 55 students. Two hundred thirty-six students are enrolled in the first two years of the program in Australia. In New Orleans, there are 122 students in their third year and 100 in their fourth year.
Ochsner Brings Telehealth Services to Areas Across LA and MS
In 2009, Ochsner began utilizing a telestroke service to improve stroke care in rural and urban areas throughout Louisiana.
Since then, Ochsner’s telemedicine program, CareConnect 360, has partnered with 41 facilities across Louisiana and Mississippi, has impacted over 550,000 patients and has now expanded its services to 32 specialties including cardiology, pediatrics, psychiatry and maternal fetal medicine.
In 2015, Ochsner completed over 135,000 telemedicine consults with other hospitals, providing stroke care, cardiac care, high-risk women's services and advanced interpretation services, among other capabilities that other hospitals may not have locally.

Community Outreach Focuses on Wellness for All Ages
The "Change the Kids, Change the Future" program focuses on nutrition, exercise and healthy eating habits, all of which set the stage for children's ongoing behavior. This fully integrated school approach encompasses education and lifestyle changes for students, staff and families to improve the health of the next generation.
Beginning in January 2013, the CHOP afterschool program (Cooking-up Healthy Options and Portions) was implemented in two Jefferson Parish middle schools by Ochsner Health System as part of its “Change the Kids, Change the Future” program and through a grant from the Humana Foundation.
By the Numbers
- In 2000, Ochsner surgeons performed the 500th heart transplant, one of only 6 U.S. transplant centers to have achieved this milestone.
- In 2002, patient satisfaction scores for the Emergency Department averaged 98 percent.
- In 2003, 456 medical students chose Ochsner for clinical training.
- The research program developed 550 new treatment protocols in 2008.
- In 2008, Ochsner experienced a 40% increase in international patients, delivered a record 5,565 babies, developed 550 new treatment protocols through our research program and saw a 30% increase in patients being transferred to Ochsner from other hospitals and health systems through our Regional Transfer Center.
North Shore Regional Medical Center Joins Ochsner Health System
North Shore Regional Medical Center joined Ochsner Health System, becoming Ochsner Medical Center - North Shore. This 165-bed acute care, full-service hospital located in Slidell, La. employs 100 physicians, more than 700 employees and has the region's only Pediatric Intensive Care Unit.

Ochsner Creates Haitian Relief Fund
Ochsner created the Haitian Relief Fund in January 2010 as a response to the devastating earthquake that occurred in Haiti on Jan. 12, 2010. Registering 7.0 on the Richter scale, the earthquake killed over 200,000 and left over 600,000 injured or homeless and struggling to find the basic resources needed for survival.
Ochsner West Bank Regional Medical Director Yvens Laborde, MD, a native of Haiti, was a driving force behind the project.
Through funds raised for the Ochsner Haitian Relief Fund, Laborde, along with other Ochsner medical personnel, are able to establish an ongoing healthcare relationship between Ochsner and the town of Maya La Victoire in northern Haiti. The fund is also instrumental in constructing a health clinic within a school; installs a water well that provides clean water for the clinic and school; provides books, uniforms, supplies and lunch for students; and provides support for teacher salaries.
As part of its partnership with University of Queensland Medical School in Australia, medical students studying locally at Ochsner Medical Center are able to participate in the work in Haiti.

Gayle and Tom Benson Cancer Center Opens
Overlooking the Mississippi River on the Ochsner campus between River Road and Jefferson Highway in New Orleans, the Gayle and Tom Benson Cancer Center features 40 infusion stations and treated 2,200 cancer patients during its first year of operation.
In 2015 alone, the center cared for 27,000 cancer patients from 42 states across the nation and 16 countries around the world.

Leukemia, Blood and Marrow Transplant Program Introduced
Bringing together highly-experienced transplant specialists, Ochsner’s new Leukemia, Blood, and Marrow Transplant Program provided a dedicated inpatient unit and outpatient infusion suite, state-of-the-art stem cell processing lab and clinical trials. In 2013, the program received internationally-recognized accreditation by the Foundation for the Accreditation of Cellular Therapy (FACT).

Ochsner Campuses Go Completely Tobacco-Free
Dr. Alton Ochsner made history in the 1930s when he became one of the very first to discover the connection between tobacco use and lung cancer. Since that time, lung cancer has risen to its current position as the second most common cancer among men and women in the United States and the leading cause of cancer deaths. Each year, more people die of lung cancer than of colon, breast and prostate cancers combined.
As a leader in healthcare, Ochsner has vigorously supported efforts to reduce tobacco use and warned the public about the very real consequences of smoking. That's why all Ochsner locations became completely tobacco-free in 2011.

Ochsner Opens State's Only e-Intensive Care Unit
Ochsner formed an agreement with Philips VISICU to implement a state-of-the-art eICU program to enhance critical care by connecting Ochsner's bedside care teams with off-site critical care physicians and nurses using continuous remote monitoring technology. This is a program that has been proven to reduce complications, shorten hospital length of stay and save lives.
As the only healthcare provider in Louisiana with the eICU program, Ochsner serves as a statewide resource to community and rural hospitals which can benefit from expanded critical care staffing and technology.

Ochsner Extends Global Reach Through Education
Ochsner partnered with King Abdulaziz University and the University of Tabuk System in Saudi Arabia. This invaluable partnership provides training and education to students, highlighting Ochsner’s connection with the international medical community.

Ochsner Installs Epic Software
Ochsner installed Epic software – combining 38 separate health record programs into one integrated Electronic Health Record. By the close of 2012, Epic had been rolled out to nearly all Ochsner outpatient clinics on the north and south shores of Lake Pontchartrain. In 2013, Epic was implemented at nearly all remaining OHS hospitals. In 2014, OHS completed the rollout by deploying Epic at Leonard J. Chabert Medical Center and upgrading the entire system to the newest, most efficient version of the software.

First Total Artificial Heart Implant in Gulf South Performed at Ochsner
The John Ochsner Heart and Vascular Institute at Ochsner Medical Center performs the first Total Artificial Heart (TAH) implant in the Gulf South Region. The latest advancement in mechanical heart technology, the Syncardia TAH is the world’s first and only FDA-approved device.

Multi-Specialty Team Performs First In-Utero Surgery in Gulf South
Ochsner Medical Center's fetal surgery team of 18 physicians and nurses operated on a 23-week-old fetus while still in his mother's uterus, a procedure that fewer than 10 hospitals in the United States are able to perform.

Ochsner Takes on Public/Private Partnership with Chabert Medical Center
Since 1978, Leonard J. Chabert Medical Center has been caring for the underserved in the region. In May 2013, a public/private partnership between Ochsner Health System, Terrebonne General Medical Center and Chabert was initiated to develop sustainable solutions to deliver these crucial safety-net services for the region while achieving unprecedented access, service, and quality of care for its patients and preserving academic training at Chabert.

Ochsner Takes on First Management Operation in Mississippi
Hancock Medical Center, a not-for-profit hospital, was Ochsner's first management operation in Mississippi. In September 2013, Ochsner signed an interim management agreement with Hancock, followed by a formalized agreement extended for two years. Today, Hancock Medical is 47 beds strong. A dedicated group of more than 100 physicians representing a broad spectrum of medical specialties make up Hancock Medical Center’s active and consulting medical staffs.

Ochsner Transplant Institute Sets Record
The Ochsner Transplant Institute reached an exciting milestone by performing its 5,000th transplant – a living kidney transplant between two family members. Established in 1984, Ochsner Transplant Institute has accomplished numerous “first” achievements including the first adult heart, pediatric heart and liver transplants in the Gulf South as well as the first double lung, kidney, liver and dual organ (kidney-pancreas) transplants in Louisiana.
CareChex® recognized Ochsner as number one in the nation in liver transplantation and number two in kidney transplantation.

Ochsner Footprint Expands Through Strategic Partnerships
Terrebonne General Medical Center
Building on its existing relationship, Ochsner and Terrebonne General Medical Center have created greater opportunity to focus on shared savings and decrease the overall cost for patients while maintaining exceptionally high quality care.
St. Charles Parish Hospital
An affiliation with St. Charles Parish Hospital further allowed Ochsner to build upon an existing relationship - including Ochsner's Telestroke program, Neurology and Primary Care services - and more fully aligned to strengthen current resources and expand access to services in the community.
River Parishes Hospital
By operating River Parishes as an outpatient medical facility and emergency room, Ochsner ensured that essential services remained available locally and that patients have access to Ochsner's nationally recognized care when they need it.

Ochsner and St. Tammany Parish Hospital Form Partnership
The Ochsner and St. Tammany Parish Hospital partnership created the most comprehensive healthcare network in western St. Tammany Parish. The two organizations announced several programs for which growth and development in western St. Tammany is a priority, including pediatric subspecialty care, comprehensive neurosciences care such as stroke care and neurosurgery, and an expansion of cardiovascular and thoracic programs.
Remembering Dr. Frank Riddick, Jr.
On Oct. 28, Dr. Frank Riddick, Jr., passed away at the age of 85. This was a significant loss not only for the Ochsner family but for the local community and for the national healthcare industry. Dr. Riddick joined Ochsner in 1961 and was a physician who spent his entire professional career here.
Honored with the Ochsner Lifetime Achievement Award in 2007, he was someone who touched many lives over the course of his tenure - both patients and colleagues. Dr. Riddick was a long-time leader at Ochsner. In addition to maintaining an active Endocrinology and Metabolic Diseases practice, Dr. Riddick served in many leadership roles and made significant contributions in helping to build the Ochsner we know today.

O Bar Uses Interactive Health Technology to Enhance Patient Engagement
Ochsner Health System was the first in the country to introduce the concept of a ‘genius bar’ in a health setting. The O Bar shared physician-recommended health apps at its state-of-the-art iPad® bar. Patients with diabetes, high cholesterol or who need help quitting smoking could test the best apps to manage their health and wellness.
The O Bar also carried the latest in cutting-edge, interactive health technology that work via a smartphone or online app, such as blood glucose monitors and scales that email daily results directly to your physician and a wireless blood pressure cuff that can plug into your phone.

Ochsner Launches Innovation Ochsner and Partners with GE for Annual Challenge
At the Health Innovation Summit at New Orleans Entrepreneur Week (NOEW), Ochsner Health System announced the launch of an innovation accelerator called iO designed to support and partner with companies working to revolutionize patient-centered care. Through the accelerator, patient-centered care solutions for both patients and providers can be tested, validated, funded and launched.
The new accelerator will focus on developing entirely new ways for providers to manage patient conditions more effectively and efficiently and empower patients via big data analytics and emerging technology. Patients using these new digital health tools including their own social media networks will be able to take an active role in monitoring, maintaining and enhancing their own health.
Ochsner and GE Healthcare announced their three-year commitment to The Idea Village as co-sponsors of what will become an annual Healthcare Innovation Summit. The Summit introduced a multi-year innovation challenge, providing resources to local entrepreneurs to catalyze new ideas within the medical industry. Each year’s theme will tackle some of the healthcare industry’s toughest challenges, with the first year focused on transforming health outcomes with ‘wearable’ technology.

Ochsner Manages Chronic Diseases with Apple Watch
The Apple Watch was used to enhance the effectiveness of the Ochsner Hypertension Digital Medicine Program, a pilot program that tracked several hundred patients struggling to control their blood pressure. Through the Apple Watch, patients received medication reminders which include actual pictures of the pill; feedback from clinicians about potential side effects once a new medication is prescribed; renewal notification for prescriptions, and activity tracking and exercise reminders.

Ochsner Health Network Formed
St. Charles Parish Hospital - and currently comprised of five of the highest quality partners – including St. Tammany Parish Hospital, Lafayette General Health, CHRISTUS Health Louisiana and Terrebonne General Medical Center - that encompass 25 facilities across the state and ultimately the region, the Ochsner Health Network provided an opportunity to come together around a common goal – our patients.
More Strategic Partnerships Expand Ochsner's Reach
Strategic partnerships have brought together some of the highest quality organizations in Louisiana. Ochsner Health System partnered with Lafayette General and CHRISTUS Health Louisiana around a shared commitment to continuously improve quality and increase local access to care while significantly reducing healthcare costs for patients across our state. Similar letters of intent were signed with Slidell Memorial Hospital and Terrebone General Hospital.

Ochsner Health System Announces $360 Million Expansion to Jefferson Highway Campuses
Ochsner Health System announced a $360 million expansion to its Jefferson Highway campus.
“The increasing number of patients transferred from facilities within and outside of the Ochsner system along with the expansion of the Ochsner Health Network, underline the growing demand for the specialty care offered here at Ochsner Medical Center,” said Warner Thomas, CEO and President, Ochsner Health System. “We are building on our legacy as a national and global destination for healthcare for the Greater New Orleans Region and the Gulf South. The next chapter is to create a more comprehensive Healthcare Corridor anchored by Ochsner Medical Center so we can continue to change and save more lives.”
The expansion of the “South Campus,” the main hospital, will increase capacity to offer more specialty care services, such as cancer care, organ transplants, neurologic, pediatric and cardiac care.
On the “North Campus”, directly across the street from the hospital, a new imaging center will offer comprehensive imaging services including CT Scans, Mammography, three additional MRI machines and more.
The newly, created “West Campus” totals 8 acres and will include the new Ochsner Rehabilitation Hospital and the Ochsner Outpatient Physical and Occupational Therapy Clinic.

Ochsner Joins the White House Precision Medicine Initiative Summit
Ochsner Health System joined President Obama as a participant in the White House Precision Medicine Initiative Summit in Washington, D.C. The Summit marks the one-year anniversary of the Precision Medicine Initiative which focuses on enabling a new era of clinical care through research, technology, and policies that empowers patients, researchers, and providers to work together toward development of individualized care.
Ochsner was one of nearly 50 organizations, including the Bill & Melinda Gates Foundation, Harvard Medical School and The Advisory Board Company, selected nationwide based on their ongoing commitment to accelerate precision medicine.

Ochsner Baptist Third Institution in Nation to use Groundbreaking Treatment for Chronic Headaches
Ochsner Baptist's Comprehensive Headache Center was the third center in the country to perform Iovera Cryotherapy, an innovative, nonsurgical procedure for debilitating headache pain called occipital neuralgia.
It is estimated that millions of Americans suffer from some form of chronic headache.
Iovera works through injections in the nerves on either or both sides of the neck and head by temporarily degenerating the nerves through a freezing process. There are no chemicals or medications, just an ice-tipped needle.

By the Numbers
- In 2010, Ochsner's 8 hospitals and 38+ health centers treated more than 336,000 unique patients from over 26 countries while employing more than 850 physicians and 12,500 employees.
- By 2014, that number had increased to nearly 400,000 patients from more than 90 countries.
- In 2014, Ochsner surpassed the 200,000 mark for patients enrolled in the MyOchsner patient portal.
- In 2014, Ochsner participated in 740 clinical studies; new patient clinical trial enrollment has seen a more than 237% increase over 2012.

Dr. John Ochsner Discovery Health Sciences Academy
In 2019 Ochsner announced one of the most meaningful and impactful community initiatives in our history — one that will benefit children, their families and the broader community for years to come. Our partnership with the Discovery Health Sciences Academy — a high-performing, open enrollment, tuition-free charter school with three campuses in Jefferson Parish — will make it possible to establish a new K-8 public charter school in the heart of the historic Shrewsbury community. It is located near Ochsner Medical Center — Jefferson Highway and it welcomed its first students in August 2020, it’s named the Dr. John Ochsner Discovery Health Sciences Academy at the John Martyn Campus.

Ochsner and Lafayette General: A Powerful Force for Health
After several years of collaboration, the bonds between Ochsner and Lafayette General Health (LGH) grew stronger in 2019 through a letter of intent for the two organizations to merge. The combination creates the largest and most comprehensive healthcare provider in the Gulf South with a focus on expanding access to high-quality care and improving the long-term health and wellness of communities across the region.

A Historic Milestone in Transplant Medicine
It was a historic event — and would set Ochsner on a path to become a leader in transplant medicine. Nearly a half-century later, in 2019 Ochsner achieved another historic milestone when a multidisciplinary team of physicians, nurses and medical professionals from the John Ochsner Heart and Vascular Institute (JOHVI) and the Ochsner Transplant Institute performed Ochsner’s 1,000th heart transplant. With the successful completion of this procedure, Ochsner became only the 14th provider in the nation to reach 1,000 heart transplants — joining Cleveland Clinic, Duke University, Vanderbilt University Medical Center and the University of Pennsylvania in this achievement.
Vision for a Healthy State
Ochsner Health welcomed 2020 with a name change and a bold new 10-year vision and commitment to create a Healthy State. Together with state leaders, community partners, insurers, schools, employers and others, we are placing a direct focus on the health and wellness of the whole person and addressing the most critical health needs in our Louisiana and Mississippi communities. In 2020, we announced a $100 million investment to address health inequities and expand Louisiana’s healthcare workforce and community-based health services. These investments include the development of 15 community health centers in underserved areas across Louisiana, the creation of the Ochsner Scholars Program to address critical physician shortages in key areas, and a partnership with Xavier University to create the Ochsner Xavier Institute for Health Equity and Research (OXIHER). In partnership with OXIHER and broad-based statewide and regional coalitions, The Healthy State Partnership will focus on these five pillars of a healthy state:
- Health outcomes & interventions
- Community wellness
- Social determinants
- Health access
- Workforce development & addressing economic disparities

Building Better Futures for Today's Boys with Son of a Saint
Ochsner’s work to build healthier communities takes many forms — and one of the most important is our sustained support for community-based programs that share our commitment to change and save lives. In 2020 Ochsner Health deepened that commitment with a new, five-year pledge of $1 million to Son of a Saint, a nonprofit organization dedicated to transforming the lives of fatherless boys in New Orleans while also inspiring mentorship. Ochsner’s support for Son of a Saint will fund critical programmatic staff and enhance the organization’s services to promote the whole person — mind, body and spirit — through healthcare educators, social workers and mental health providers. It will also provide opportunities for Ochsner’s male staff to mentor boys in the program. Noted Ochsner President and CEO Warner Thomas, “Our partnership with Son of a Saint is not only a monetary donation, but also an investment in the health, wellness and future of the young men of New Orleans.”

A Meaningful Milestone in the Fight Against COVID-19
Just over a month after Ochsner Medical Center — New Orleans admitted its first COVID-19 patient, the hospital reached an important milestone with the discharge of its 1,500th patient. On April 20, patient Kathleen Bennett was cheered by scores of hospital staffers and serenaded by a musician as she was wheeled out of the hospital by Ochsner RN Dominique Yancey. During such a challenging time for patients and staff, it was finally a cause for celebration.
We Believe: Deeping Ochsner’s Commitment to Diversity, Equity and Inclusion
- Even as Ochsner employees worked on the front lines battling COVID-19, providing expert, compassionate care to thousands of patients while helping communities strengthen their response to the pandemic, there was another crisis that impacted all of us in 2020: social unrest and the fight for racial justice. While Ochsner’s commitment to diversity, equity and inclusion (DEI) is not new, the events of the year brought into sharper focus the opportunities to raise our goals, expand our initiatives and strengthen our workplace culture — work that we undertook with a sense of passion and urgency.
A broad spectrum of DEI accomplishments highlighted the year, beginning with the hiring of Ochsner’s first Chief Diversity Officer, Deb Grimes. Working in collaboration with other senior Ochsner leaders and our Board, Deb and her team deepened employee engagement around DEI goals and objectives, expanded training programs and implemented new measures to advance our supplier diversity goals. Included among the year’s achievements:
- Grew the number of Ochsner Resource Groups (ORGs) to eight, adding two new ORGs created for Asian-American and Pacific Islander staff and for those with disabilities.
- Formed Ochsner’s first System DEI Leadership Council comprised of ORG presidents, system leaders and Board members.
- Hired Ochsner’s first DEI team members, including nine regional directors to align system and local strategies, and team members to manage the ORGs and the supplier diversity strategy.
- Launched DEI education and training programs across the system, including those focused on unconscious bias, which attracted significant levels of employee participation.




















