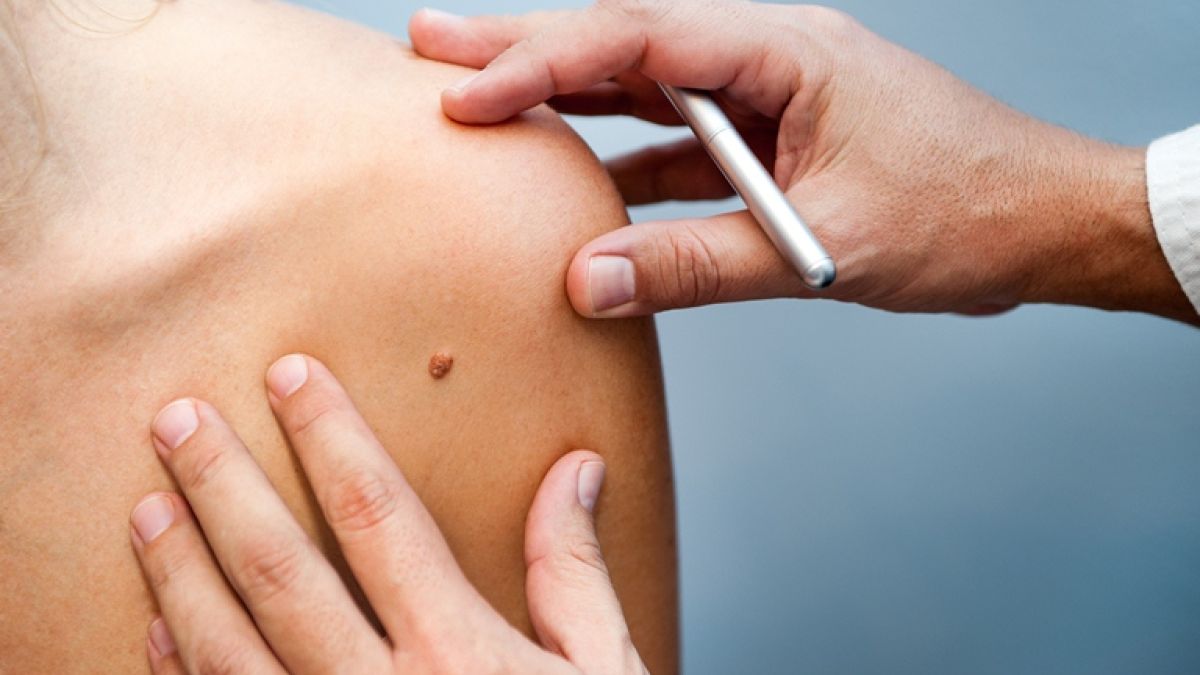
Melanoma is an aggressive type of skin cancer. It is the least common type of skin cancer overall but is the most common in children. Overall, it is a rare cancer, with only ~75,000 cases in the US per year, but has become more common over the past several decades, presumably due to increased ultraviolet (UV) light exposure. The most common cause of melanoma is UV light. People with fair skin are more likely to develop melanoma. At Ochsner Children’s, our Pediatric Oncologists work with a multidisciplinary team to provide state of the art care to children and young adults diagnosed with melanoma. This includes pediatric oncologists, pediatric dermatologists, radiation oncologists, and pediatric surgeons. We are very active in research and clinical trials designed to increase cure rates, decrease treatment-related side effects and improve care for long-term survivors.
Ochsner Health is the leading nonprofit healthcare provider in the Gulf South. Ochsner inspires healthier lives and stronger communities through our mission to serve, heal, lead, educate and innovate.